I am a senior physician with over six decades of experience who has observed his share of critical illness—but only from the doctor’s perspective. That changed suddenly and disastrously on the morning of June 27, 2013, ten days after my ninetieth birthday, when I fell down the stairs in my home, broke my neck, and very nearly died. Since then, I have made an astonishing recovery, in the course of which I learned how it feels to be a helpless patient close to death. I also learned some things about the US medical care system that I had never fully appreciated, even though this is a subject that I have studied and written about for many years.
As background, I should first explain that this was not my first experience as a patient. Over the years I had acquired a multitude of ailments common to the elderly, most of which were minor. However, I have a few more serious health problems, including long-standing atrial fibrillation (an irregularity of my heart rhythm) that requires the daily administration of warfarin, an anticoagulant drug, to prevent the formation of blood clots inside my heart. More recently, I developed aortic stenosis, a slowly progressive narrowing of the heart valve that controls the outflow of blood into the aorta. So far, it has not caused any cardiovascular symptoms, but it could do so at any time.
And some four years ago, I developed a mysterious and very painful disorder of the muscles and joints, called polymyalgia rheumatica, relieved only by the daily administration of prednisone. This disorder, combined with an unsteady gait (caused by a viral infection of my inner ears many years ago), made it necessary to walk with a cane, and difficult to climb the stairs in my multilevel condo. For this reason, a stair lift had been installed to help me navigate the first and steepest flight of stairs from our entrance hallway to the first floor.
Despite all these ailments, I had never needed more than a brief hospitalization—until that fateful morning of June 27. I was hurrying down the stairs to meet a cab that was waiting to take my son to the airport. He had been visiting from his home in Washington, D.C., while my wife was on a brief trip to Santa Fe. Neglecting to use the stair lift, I lost my balance and pitched forward, landing hard on my head on the slate floor of the hall. I heard a loud crack as my head hit the floor, and although I did not lose consciousness and felt very little pain, I knew at once that I must have sustained severe injuries.
My son heard me fall, rushed down to me, wrapped a towel around my bloody head, and helped me into the waiting cab. I told the startled driver to take us not to the airport, but to the emergency room of the Massachusetts General Hospital (MGH), where my cardiologist is on the staff, as quickly as possible. We arrived at the MGH emergency room at about 7:30 AM. I identified myself and gave a quick account of what had happened. Within a few minutes, it seemed, my cubicle filled with physicians, nurses, and other members of the staff. I can remember only a few details, but recall being taken for a CT scan and other X-ray studies.
But very quickly after that, I became short of breath and started to choke. I was told later that I exclaimed, “I need to be intubated,” while the monitoring equipment showed that my oxygen levels were plummeting. At that point I lost consciousness and did not wake until about five hours later in the surgical intensive care unit (ICU). What happened in the interval I learned partly from my son and daughter (who lives nearby and had soon joined him in the ER), but mainly from reading my medical record, which I obtained from the hospital months later.
The initial X-rays, including the CT scan, showed fractures of three vertebrae in my neck (C1, C2, and C5), as well as multiple fractures of bones in the right side of my face and part of my skull. There was also fresh bleeding on the surface of the right frontal lobe of my brain, but fortunately no evidence that the fragments of bone in my neck were impinging on my spinal cord—which was the greatest danger I faced, since a severed spinal cord at that high level would have caused immediate death or, at best, quadriplegia.
There was massive hemorrhage around the injuries, so immediate treatment included large doses of vitamin K, which offsets the anti-clotting effects of the warfarin I was taking for my atrial fibrillation and would help reduce the bleeding. Also, I was given large doses of adrenal steroids and intravenous fluids to protect against the life-threatening effect of stress, because the response of my own adrenal gland to stress had been suppressed by taking daily prednisone. In addition, a large, rigid collar (later referred to by my wife as a medieval torture device) was placed around my neck to prevent any movement that might shift the fractured vertebrae and compress the spinal cord. These initial measures undoubtedly saved my life.
Advertisement
But when I began to choke and my oxygen level fell, this signaled a new threat. The massive hemorrhage had started to compress my windpipe, or trachea, making it impossible for me to breathe. An anesthesiologist tried to get a breathing tube into my trachea, but could not—partly because of the obstruction, and partly because of the need to keep my neck immobilized. Within the next few minutes a member of the surgical trauma team, who had been urgently summoned, began to do an emergency tracheotomy. He quickly made an incision in my lower neck and was able to insert a tube into my trachea through which a mechanical ventilator could pump air.
During that procedure, the drop in blood oxygen caused my heart to stop. I would certainly have died then had it not been for the medical team, who immediately started cardiopulmonary resuscitation efforts as oxygen was being pumped into my lungs through the tracheostomy. I was also given injections of drugs to stimulate my heart. Within two minutes my heartbeat resumed, but during the next fifteen minutes or so, my heart stopped twice more—each time responding within about a minute to CPR. My cardiologist, a senior and much-respected clinician, arrived in the ER just in time to advise the team on their management of the cardiac arrests and the treatment of my rapidly changing heart rhythms and blood pressure that followed the resuscitation. The resuscitation saved my life, but as is often the case, the compression of my chest cage fractured several ribs.
After this crisis passed and my cardiac function had been stabilized, other X-rays and laboratory tests were done. A catheter was passed through a large vein at the base of my neck into the right side of my heart to monitor my cardiovascular function. Another catheter was placed in an artery in my left arm to give direct access to the arterial side of my circulation. My tracheostomy tube had already been connected to a mechanical ventilator, which assisted my breathing. In addition, a catheter was placed in my bladder to measure my urinary output. I also underwent three bronchoscopies to suck blood clots out of my bronchi and help clear my lungs.
About five hours after arriving in the ER, I was brought to the surgical ICU. Gradually awakening, I could not speak because of the tracheostomy and ventilator, but was told where I was, and what had happened. My wife and our children all gathered at the ICU very late that first night—three physicians and three lawyers, a company that in other hospitals might have bothered the hospital staff. But not here.
The doctors and nurses kept my family informed and were receptive to their questions and suggestions. For their part, my family were at my bedside as much as possible. My wife was especially comforting and stayed long hours with me. The nursing staff did everything they could to relieve my discomfort. They were always available day and night, and all of them were competent and kind. But I was constantly struggling to breathe through the emergency tracheostomy, and could not rest. It seemed as if I were trying to breathe through a narrow straw. Also, I was frequently choking on blood and secretions that accumulated in my throat and in the tracheal tube. Adding to my misery were the constraints imposed by the rigid collar around my neck and all the catheters and tubes to which I was attached.
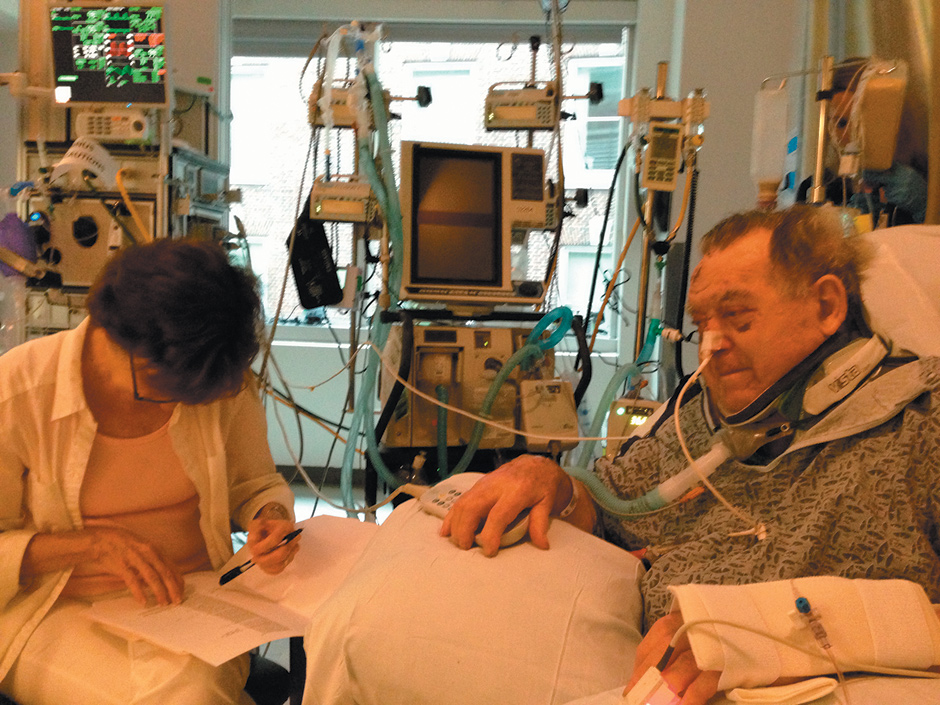
Unable to speak, I could only scribble short messages on writing pads my wife provided. During the day she would transmit my questions and requests to the nursing and medical staff. But looking over those notes, which my wife saved, I can see that constantly scribbling messages, many of which were of no conceivable importance, was my desperate attempt to maintain contact with the world. At night, when I seemed most in need of ventilatory support and suctioning of my mouth and respiratory tract, the nurses would try to understand my written requests and do their best to comply. My neck pain was often severe. I asked for the least amount of morphine to relieve it, because I wanted to remain alert. I feared morphine would suppress my respirations and increase the possibility of pneumonia. However, the record shows that in the first two or three days I received considerable sedation and morphine.
Advertisement
Despite the medication, my physical distress and utter helplessness made these first days in the ICU a terrible ordeal. I survived by concentrating on each physical problem. My life hung in the balance, as did the risk of quadriplegia, but I did not think much about these threats because I was totally concerned with relieving my immediate symptoms.
Worst of all were the endless nights. I slept very little and spent most of the time watching the minutes go by on the big wall clock in my room, waiting for daylight and the return of my wife, and other family members. They tell me that I seemed more affectionate than usual; perhaps it was because I needed them so much.
During the day I was visited on rounds by teams of physicians. They spent most of their time outside my room, studying and discussing the data on their mobile computers. Nurses also joined in the rounds, as my wife did occasionally. My primary care physician, who is on the staff of the Brigham and Women’s Hospital, a founding member of the Partners Health System along with the MGH, was kept fully informed of my condition.
The first piece of really good news came on the third day, when an MRI of my neck showed that there was no need for surgery to stabilize the fractured vertebrae. That was a great relief to the physicians in my family because they doubted I could have survived the major surgery that would have been required. The neurosurgeons continued to be concerned by a leak of cerebrospinal fluid through my nose, which they thought might require treatment by draining fluid from my lumbar spinal space. Fortunately, that leak eventually stopped on its own.

The respiratory team knew that I continued to struggle with my breathing, which required frequent assistance from the mechanical ventilator. Finally on Sunday, my fourth day in the ICU, I was taken under anesthesia to the operating room, where surgeons replaced the tracheostomy tube with a larger one that made breathing much easier. Because I could not take anything by mouth, they placed a narrow plastic tube in my stomach through my right nostril for subsequent tube feedings.
Easier breathing marked the beginning of rapid improvement. My bladder catheter soon came out, as did the central line in the right side of my heart and the arterial catheter in my left arm. Thus freed, I could begin getting out of bed and I started to walk a few steps with help. The tracheostomy tube was adjusted to allow me to start talking.
Nowadays, hospitals like Massachusetts General are mainly for the acutely sick and seriously injured and for those requiring operations and other procedures that need hospitalization. Therefore, plans were soon made to transfer me to the Spaulding Rehabilitation Hospital in Cambridge, a chronic care hospital affiliated with Partners Health System. There I could continue my recovery while receiving the medical care I still needed, in addition to physical therapy to regain my strength. So, on July 8, after eleven days in the ICU, I was transferred by ambulance to a private room on the third floor of the Spaulding Hospital, to begin what would be a month of rehabilitative treatment.
Although it belongs to the Partners Health System, the medical care at Spaulding was not well organized. I was seen often by an attending physician and an associate who covered for him on weekends and when he was on vacation. But neither physician seemed to be actually in charge of my care, or spent much time at my bedside beyond what was required for a cursory physical exam. They did, however, leave lengthy notes in the computerized record, full of repetitious boilerplate language and lab data, but lacking in coherent descriptions of my medical progress, or my complaints and state of mind. In the entire record (which I later obtained) I could find only one mention of communication by a Spaulding doctor with my primary care physician (although he tells me he was consulted twice).
The nursing care was sometimes excellent but often inadequate, and assignments were changed much too frequently. The physical and occupational therapists were the best part of the professional staff; they did a very good job of helping me to learn to walk and to exercise muscles weakened by disuse. But most of the time during the first two weeks I was unable to get out of bed or even move without help because I was still encumbered by the rigid neck brace and the feeding tube, which was connected to a bedside drip that slowly administered liquid nourishment. During this time I also developed a bedsore at the base of my right buttock, which added to my discomfort and was largely left to my wife to deal with.
My nights in Spaulding were terrible, just as they were in the MGH ICU. One of the great risks to very ill, immobilized patients is infection—mainly pneumonia, which is most likely in heavily sedated patients. Because of that risk, I was unwilling to take sedatives or sleep medication, so I lay awake most of the time watching the clock, sometimes waiting much too long for responses to my calls for help in getting up to urinate. And when I would occasionally doze off, I was soon awakened by someone coming to check my blood pressure, or by noise in the hall outside my room.
About halfway through my stay at Spaulding, I returned by ambulance to see the surgeons at the MGH who had done the emergency tracheotomy. They saw no need to keep the tracheostomy open any longer. So with my ready assent the tracheostomy tube was quickly and easily removed. About the same time—that is, about a month after the injury—the orthopedic spine surgeon decided that the fractured vertebrae were healing well enough to remove the rigid neck brace. But at my wife’s suggestion, it was replaced with a soft neck collar that could be easily removed when I was lying quietly or sitting in a chair. This was not only enormously more comfortable, but enabled me to begin swallowing small sips of water.
Near the end of my stay at Spaulding, the most critical issue concerned my ability to swallow solid foods. The team of swallowing specialists were convinced from their fluoroscopic studies that I could not swallow food without risking aspiration into my lungs. They therefore advised continued tube feeding, but recommended replacing the tube that went from my nose to my stomach with one inserted directly into my stomach through my abdominal wall (called a G-tube), which would be more comfortable. They thought it might be weeks or even a month or two before I could safely take food by mouth. But supported by other medical advice and my own conviction that removal of the nasal tube and the neck collar would enable me to swallow normally, I declined that advice, and asked for removal of the nasogastric tube and a trial of eating. My first meal, after some six weeks with only tube feedings and a loss of twenty-five pounds, was a plate of scrambled eggs with thickly buttered toast and a glass of milk. I had no problem swallowing, then or thereafter.
I left Spaulding on August 5 to move with my wife into a furnished one-floor apartment near the MGH, which she had rented for a month. It was arranged for me to get frequent physical therapy in the apartment, while an extended stair lift was installed in all levels of our condo. We finally returned home at the end of August, ten weeks after the accident.
Fortunately, my mental functions seem to have remained intact. My ability to read, think, speak, and write is essentially unchanged, so far as I can tell. Not so for my emotional state, which has clearly changed. I do not fit the description of that currently popular diagnosis, PTSD (post-traumatic stress disorder), nor do I think a psychiatrist would call me “depressed.” But I certainly have been sobered by the realization of the fragility of my existence and my limited future.
With my physical recovery, my enjoyment of classical music and my interest in reading and current affairs, totally absent during the first two months, have all returned. I now listen to the music I love and I think a lot about the future of our country and the world.
What did this experience teach me about the current state of medical care in the US? Quite a lot, as it turns out. I always knew that the treatment of the critically ill in our best teaching hospitals was excellent. That was certainly confirmed by the life-saving treatment I received in the Massachusetts General emergency room. Physicians there simply refused to let me die (try as hard as I might). But what I hadn’t appreciated was the extent to which, when there is no emergency, new technologies and electronic record-keeping affect how doctors do their work. Attention to the masses of data generated by laboratory and imaging studies has shifted their focus away from the patient. Doctors now spend more time with their computers than at the bedside. That seemed true at both the ICU and Spaulding. Reading the physicians’ notes in the MGH and Spaulding records, I found only a few brief descriptions of how I felt or looked, but there were copious reports of the data from tests and monitoring devices. Conversations with my physicians were infrequent, brief, and hardly ever reported.
What personal care hospitalized patients now get is mostly from nurses. In the MGH ICU the nursing care was superb; at Spaulding it was inconsistent. I had never before understood how much good nursing care contributes to patients’ safety and comfort, especially when they are very sick or disabled. This is a lesson all physicians and hospital administrators should learn. When nursing is not optimal, patient care is never good.
Even in the best of hospitals, with the best of medical and nursing care, the ICU can be a devastating psychological experience for patients—as it was for me. Totally helpless, deprived of control over one’s body, ICU patients desperately need the comforting presence of family and loved ones. I was fortunate to have that support, but some others in the MGH ICU were not. I can only hope they received extra attention from their nurses.
My experience at Spaulding was much different from that at MGH, and the lack of integration of its facilities to deal with particular cases was more typical of the US health system. Spaulding illustrated how patients, even when they are physicians, can feel adrift and confused when their care lacks firm, identifiable coordination by a physician in charge, to whom the patient can look for guidance and information. That function is best performed by the patient’s own primary care physician, but sometimes a hospital specialist can play that part just as well.
What is important is that someone who knows the patient oversees their care, ensures that the many specialized services work together in the patient’s interest, and that the patient is kept fully involved and informed. At Spaulding, that was not the case, and the US health care system suffers from the same deficiency. The growing national shortage of primary care physicians allows for fragmentation, duplication, and lack of coordination of medical services. However, despite Spaulding’s problems and my concerns, I did improve while there, and I left the institution in much better shape than on arrival.
So far, I have said nothing about costs, although costs are the central problem for our medical care system, and my care was very expensive. Fortunately, I was well insured through Harvard’s faculty plan, which covered almost all of my medical expenses. The plan was charged $330,000 for my eleven days at MGH, and $76,000 for my month at Spaulding. Neither of these charges was itemized. In addition, the plan was charged $69,000 for physicians’ services and special procedures, and $3,000 for ambulance service. After reviewing these charges and discounting some of them as excessively high, the Harvard plan paid a total of $332,000, leaving me with only a few hundred dollars in copayments for physicians’ care. Had I relied instead on Medicare, I estimate that the same services would have cost me a few thousand dollars for deductibles and copayments.
Medicare’s rising costs are a serious drain on the federal budget, and very elderly beneficiaries like me are responsible for a major part of that expense. Given the limited life expectancy of someone my age, is it justified to spend hundreds of thousands of dollars to extend a nonagenarian’s life a little longer? That is a question needing more discussion than I can undertake here. I would hardly be an unbiased voice, since it was my life that was at stake, and I was very glad it was saved. Of course, in our health system, charges may have little relation to true costs, making such a discussion still more difficult to pursue.
Just a few months after very nearly dying, I am beginning to resume my previous activities and enjoy my life again. However, I walk slowly with a cane, and my movements are deliberate and more cautious to avoid any more falls. My astonishing recovery would never have happened without the superb emergency treatment I received at the MGH and the rehabilitative care that followed. But I am also convinced that other factors contributed to my survival: my family’s support (particularly that of my wife), a strong body, an intact brain, and very good luck all were important. I also believe my medical training helped. It made me aware of the dangers of pneumonia and other infections from contamination of catheters and tubes, so I pushed to have the latter removed as soon as possible and I took as few sedatives and painkillers as possible.
However, there was something else that helped to sustain me. I wanted to stay around as long as possible to see what was going to happen to my family, to the country, and to the health system I was studying so closely. Perhaps I was too engaged in life to allow death to intrude right then. As I wrote to my wife in one of my myriad scrawled notes the first week in the ICU, “I intend to hang around for a while longer, to love and bother you.”
This Issue
February 6, 2014
The Whistleblowers
The Most Catastrophic War