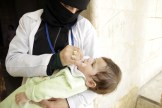
Health Care Under Fire
The fight to protect medical and humanitarian workers is not new, but we are running out of time before it becomes futile.
Perilous Medicine: The Struggle to Protect Health Care from the Violence of War
by Leonard Rubenstein
Necessary Risks: Professional Humanitarianism and Violence Against Aid Workers
by Abby Stoddard
June 23, 2022 issue